Important Facts About Hyperthyroidism & Related Problems
- 1 Oct, 2015
- Written by Team Dr Lal PathLabs
Medically Approved by Dr. Shuchi
Table of Contents
INTRODUCTION
Hyperthyroidism, also known as Thyrotoxicosis, is the clinical syndrome that results from elevated concentrations of free thyroid hormone in the plasma, associated with clinical evidence of hypermetabolism.
CAUSES
GRAVE’S DISEASE (GD)
- GD is overall the most common cause of Hyperthyroidism. GD is caused by a generalized over activity of the entire thyroid gland (Hyperthyroidism).
- GD is an autoimmune disorder in which Thyroid Receptor Antibodies (TRAbs) stimulate the TSH receptor, increasing thyroid hormone production.
Prevalance
Women are more frequently affected by Grave’s Disease than men by a 5:1 ratio. TRAbs are present in 70-100% of Grave’s Disease (85-100% for activating antibodies and 75-96% for blocking antibodies).
The prevalence of hyperthyroidism has been studied in several studies in India.
- In an epidemiological study from Cochin, Subclinical and Overt Hyperthyroidism were present in 1.6% and 1.3% of subjects participating in a community survey.
- In a hospital-based study of women from Pondicherry, Subclinical and Overt Hyperthyroidism were present in 0.6% and 1.2% of subjects.
Pathogenesis
The Hyperthyroidism of Grave’s Disease is caused by Thyroid stimulating immunoglobulin that are synthesised in the thyroid gland as well as in bone marrow and lymphnodes. A combination of environmental and genetic factors, including polymorphism in HLA- DR, CTLA-4, CD25, PTPN22 & TSH-R contribute to Grave’s Disease susceptibility. Cytokines appear to play a major role in thyroid-associated opthalmopathy.
Clinical Manifestations
Laboratory Evaluations
In Grave’s Disease, the TSH level is suppressed & total and unbound thyroid hormone levels are increased. In 2-5 % of patients, only T3 is increased (T3 toxicosis).
Measurement of Thyroid receptor antibodies is the most reliable diagnostic method if the diagnosis is unclear clinically.
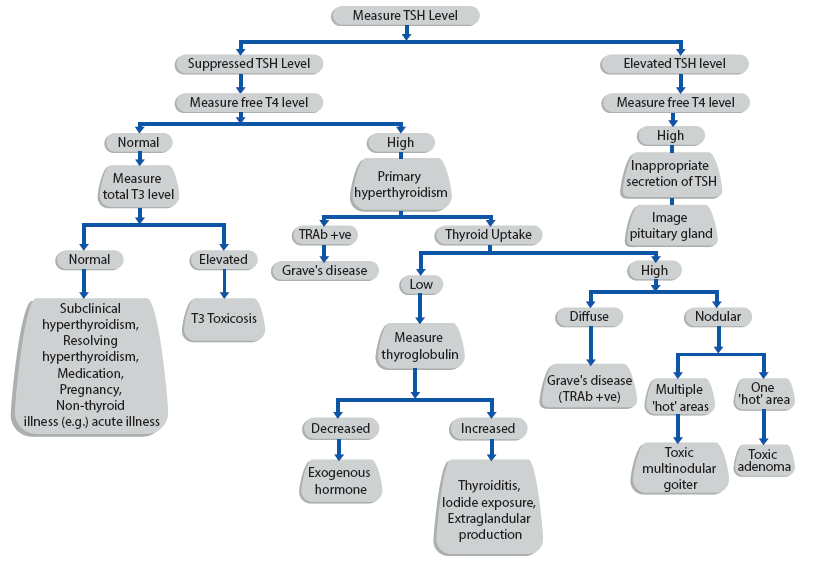
A SCHEME FOR EVALUATING SUSPECTED
HYPERTHYROIDISM
HYPERTHYROIDISM IN PREGNANCY
Graves’ disease is the most common cause of autoimmune hyperthyroidism in pregnancy, occurring in 0.1%–1% (0.4% clinical and 0.6% subclinical) of all pregnancies. More frequent than Graves’ disease as the cause of thyrotoxicosis is the syndrome of gestational hyperthyroidism defined as ‘‘transient hyperthyroidism, limited to the first half of pregnancy characterized by elevated FT4 and suppressed or undetectable serum TSH, in the absence of serum markers of thyroid autoimmunity’’ . It is diagnosed in about 1%–3% of pregnancies, depending on the geographic area and is secondary to elevated hCG levels. Determination of TSH receptor antibody (TRAb) is indicated for differentiating gestational hyperthyroidism from Grave’s hyperthyroidism in pregnancy.
Fetal risks for women with active Graves’ hyperthyroidism are 1) fetal hyperthyroidism, 2) neonatal hyperthyroidism, 3) fetal hypothyroidism, 4) neonatal hypothyroidism, and 5) central hypothyroidism.
Recommendation
If the patient has a past or present history of Graves’ disease, a maternal serum determination of TRAb should be obtained at 20–24 weeks gestation for determining the risk of Neonatal Thyrotoxicosis.
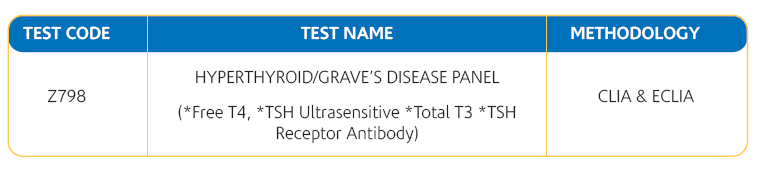
TEST RANGE AVAILABLE
CLINICAL REFERENCE
- Harrison’s Principles of internal Medicine, 18th Edition
- Guidelines of the American Thyroid Association for the Diagnosis and Management of Thyroid disease during Pregnancy & Postpartum, 2011
- Tietz Textbook of Clinical Biochemistry, Fifth Edition